We turn this week to another valvular problem: mitral regurgitation. Unlike aortic stenosis, where the valve doesn’t open all the way, in mitral regurgitation (usually abbreviated “MR”) the mitral valve (sitting between the left atrium and left ventricle) doesn’t close completely, allowing blood to regurgitate backward. Physicians often describe this condition to their patients as having a “leaky valve.”
The causes of MR are somewhat more varied than aortic stenosis, but can generally be categorized into either a primary problem with the valve itself or problems with the chambers, leading secondarily to MR. In the images below, the middle two pictures represent abnormalities of the mitral valve apparatus, one being mitral valve prolapse (usually abbreviated “MVP”) where the valves are thickened and billowy and the valve doesn’t close correctly due to this abnormal structure; and the second image showing how the valve cannot close properly due to damage to the supporting structures, in this case the chords (chordae) that attach the valve to the papillary muscles in the left ventricle. In the final image is an example of “secondary” MR, where the left atrium and ventricle are dilated, stretching the scaffolding of the mitral valve (called the mitral annulus), which leads to the leaflets being pulled away from each other and not closing properly.
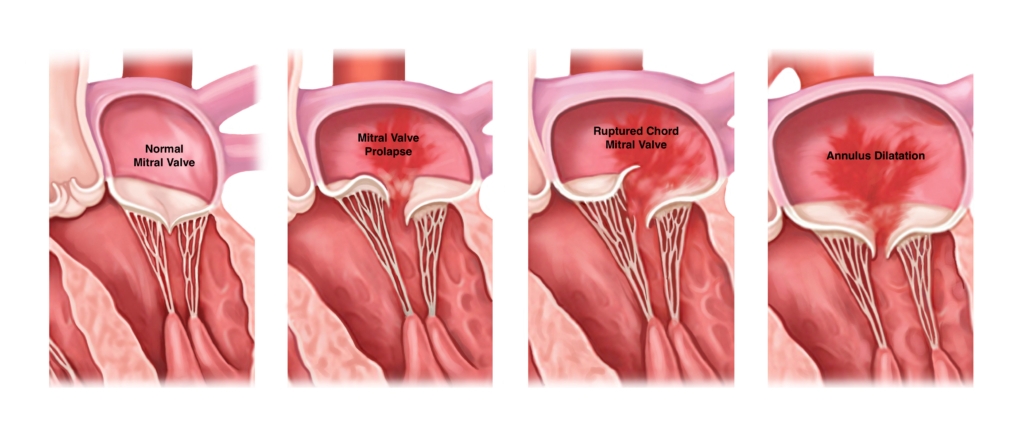
One thing to keep in mind about mitral valve prolapse—it has often been over-diagnosed, particularly in the 1990s and early part of the 2000s. A little prolapse or bowing in of the mitral valve leaflets is common. Less common are major structural abnormalities that lead to significant MR. So, if you’ve been given a diagnosis of MVP in the past, don’t assume you’re destined to have severe MR. See a cardiologist to find out if you really have a mitral valve problem or not.
Like aortic stenosis (and all valve abnormalities), we grade the degree of MR as mild, moderate or severe. Mild MR is quite common and doesn’t cause any problems. Generally, people only develop strain on their heart when the MR is severe or close to it. With that degree of regurgitation, a person can develop shortness of breath or fatigue due to the heart having to work harder to make up for the blood that is going “backward” in the circulation, as it tries to pump extra blood to compensate. Over time, this can lead to heart enlargement and weakening (“cardiomyopathy”) with congestive heart failure.
The treatment for severe MR that is associated with symptoms or compromise of the heart has traditionally involved open-heart surgery, either with replacement of the mitral valve or by repairing it. As was discussed last week with aortic valve surgery, replacement involves a prosthetic valve, either bioprosthetic or mechanical. Sometimes, in particularly skilled surgical hands, the valve can be repaired instead of being replaced.
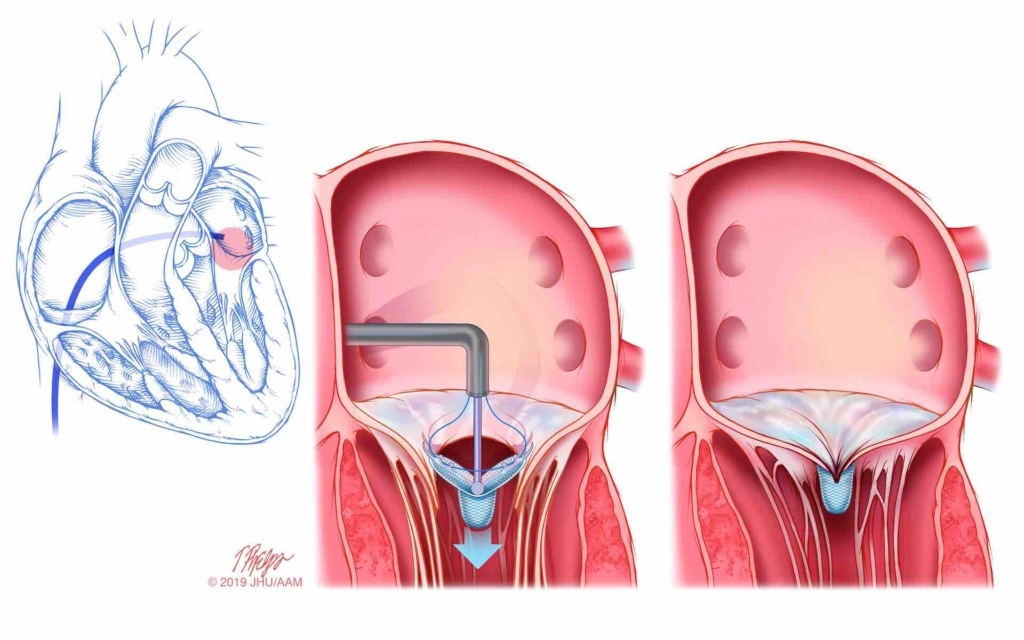
Also, like aortic stenosis, new procedures are being developed to repair the mitral valve non-surgically, using catheters. The most studied of these is the Mitral Clip, shown in the images below, where the valve has a clip placed into the center of the leaflets, helping them to close better. Patients who are too high risk for open-heart surgery now have another option to treat MR, allowing them to feel better and live longer. With the rapid pace of technologic change, even more devices and procedures will be available in the future.
Greg Koshkarian, MD, FACC
