We have spent the last couple months discussing “cardiac risk factors”: the main things that increase a person’s risk of developing coronary artery disease, also known as coronary heart disease (abbreviated “CAD” and “CHD,” respectively). We now return to consider that disease entity in greater detail.
CAD is the process of plaque accumulating in the coronary (heart) arteries (the blood vessels that supply blood to an organ). Most people have three major arteries supplying the heart with blood, but the anatomy can vary from person to person—for some people a branch vessel off a main one can be quite large and function as a “major” vessel. Plaque is a mixture of cholesterol and other lipids, inflammatory cells and molecules, and extracellular “debris.” Cardiologists often call CAD a disease of the endothelium, which is the inner lining of our blood vessels. When exposed to high blood pressure, tobacco, cholesterol, and elevated blood sugar—to name the most prominent irritants—the endothelium is injured, and this allows inflammatory cells and cholesterol to attach to and migrate inside the vessel wall (see images below). Further inflammation ensues and the plaque grows.
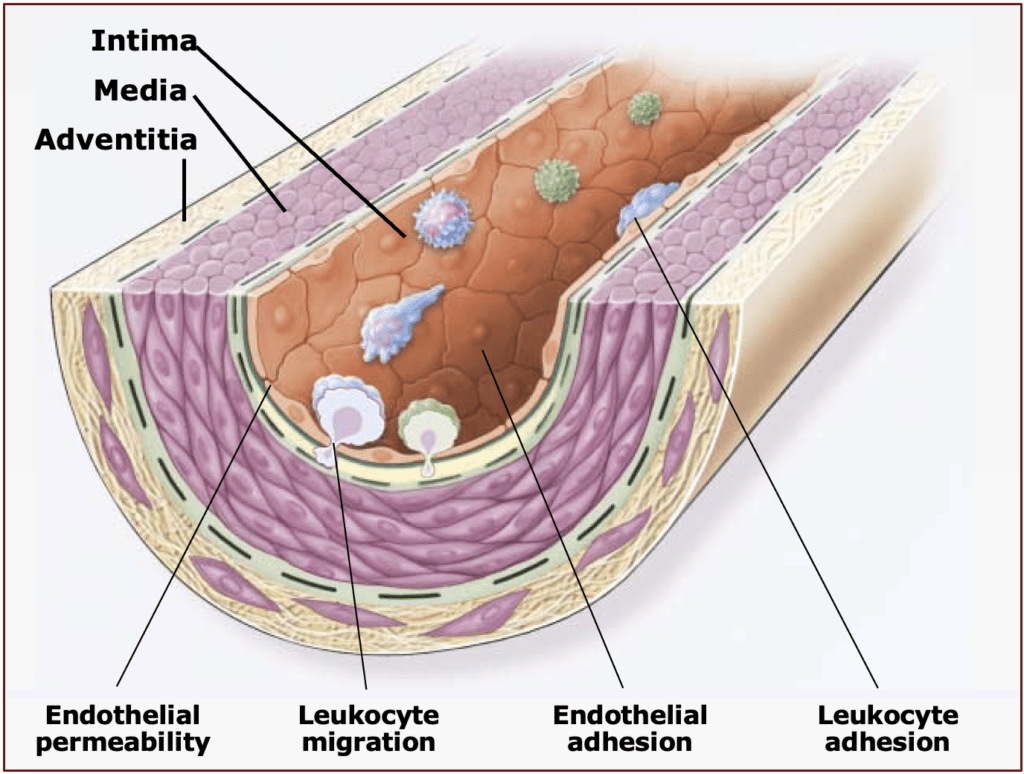
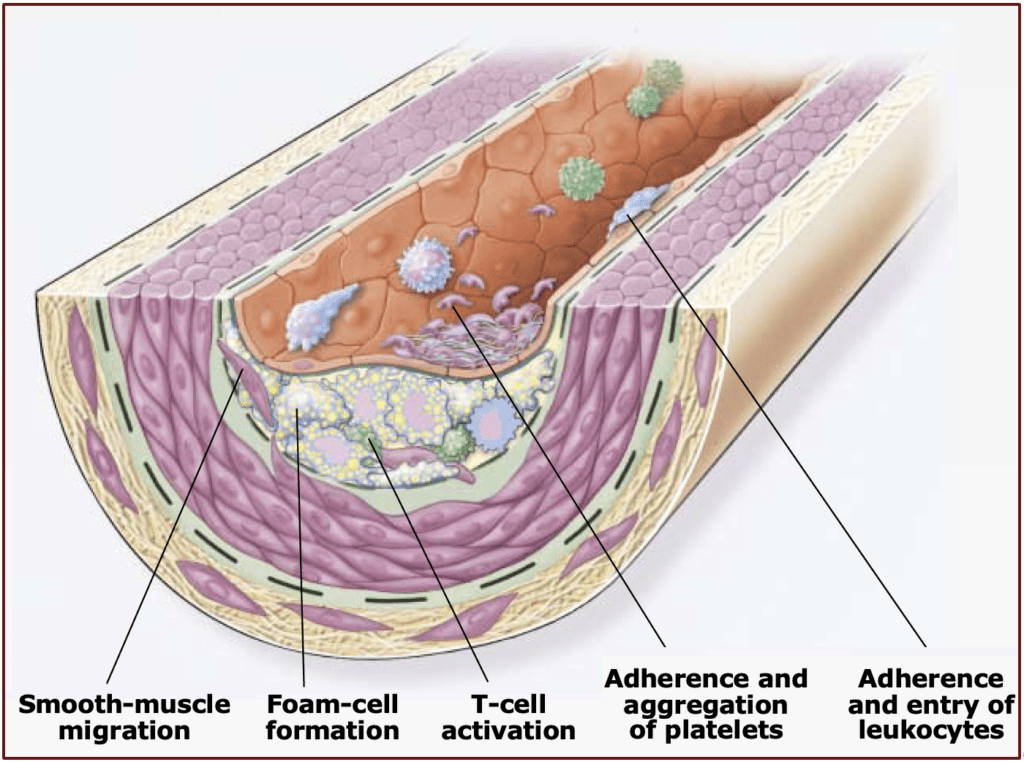
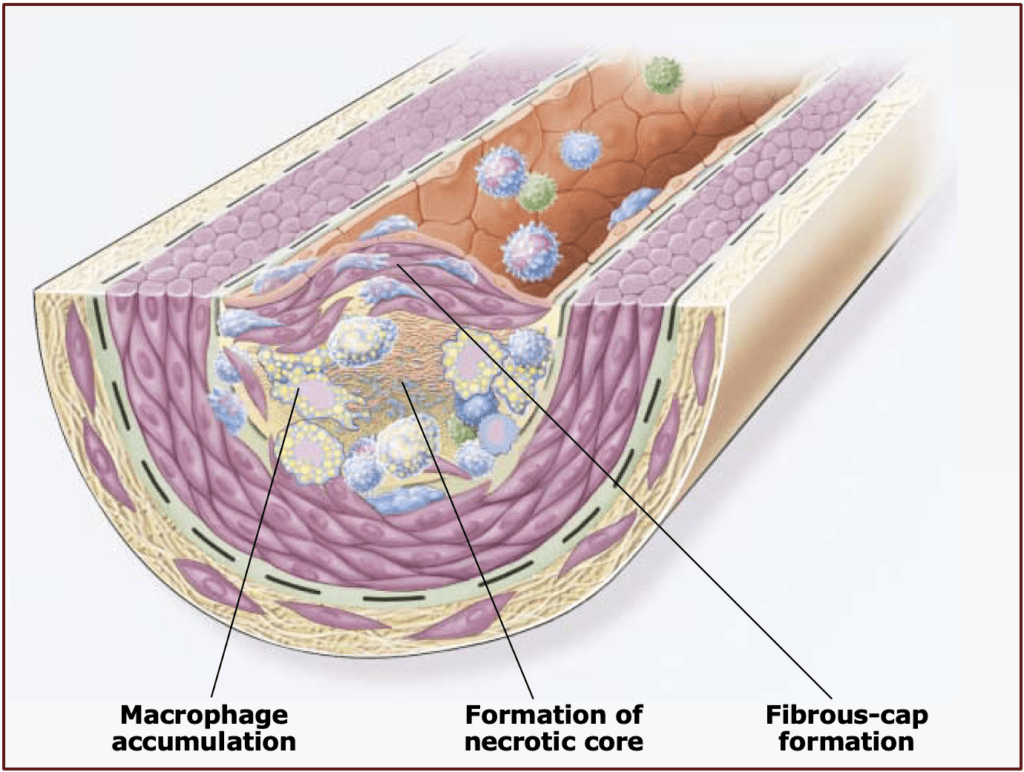
The plaque that grows in the arterial wall is, at first, accommodated by the whole vessel getting larger, a process we call vascular remodeling. This initially prevents the plaque from growing inward, which would obstruct blood flow. But over time, the vessel can no longer compensate for the enlarging plaque, which eventually grows inward into the space where blood flows: the lumen. Interestingly, by the time there is any degree of encroachment into the vascular lumen, the plaque already occupies about 40% of the cross-sectional area of the vessel (see image below).
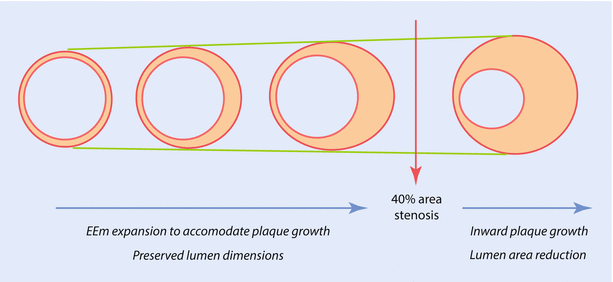
There are several things a plaque can do to cause harm. It can enlarge gradually and narrow the lumen to a point where the blood supply to that part of the heart is compromised, leading to what we call ischemia. Because the blood supply has a large reserve, a plaque needs to obstruct the lumen by more than 50-70% before the heart starts to feel starved of blood. Ischemia may be asymptomatic—but detectable on a stress test—or it can be symptomatic, leading to angina, which is usually felt as chest pressure or tightness, but can also be experienced as shortness of breath, jaw discomfort or left arm pain/heaviness/numbness.
Most people don’t realize that plaques can obstruct an artery very quickly, going from 50% to 100% in moments. This occurs when the endothelium overlying the plaque breaks, a process we call plaque rupture. In this situation, the plaque extrudes into the lumen locally and the bloodstream is exposed to the plaque components, which activates platelets and clotting factors. In a sense, the bloodstream “thinks” that the vessel has been injured and does what it has been biologically programmed to do—form a clot to wall off that vessel from the rest of the bloodstream in order to prevent life-threatening hemorrhage. However, this leads to that vessel closing off (or, if the clot is not 100% obstructive, just becoming sub-totally occluded) and causing a loss of blood flow to that part of the heart. The sudden cessation or near-cessation of blood flow to a part of the heart is what we term a myocardial infarction, also known as a heart attack. In this situation, heart muscle is irreversibly damaged.
In next week’s blog, we’ll take a look at what a person experiences when a heart attack occurs.
Greg Koshkarian, MD, FACC
